Telehealth Here to Stay, & Bringing Financial Boon
Ryan Sommers, PMP, Senior Director, Epic Practice
Jun 17, 2020

It is no secret to health clinics and medical groups that Telehealth has been a financial lifeline in 2020. And while much of that has stemmed from relaxed regulation and reimbursement expectations for COVID-19, it is also presenting a compelling argument for long-term financial strategy and sustainability. Having already garnered favor and use, Telemedicine in the United States is rocketing toward a $20B valuation this year, with steady growth expected for years to come as well.
The Long Game
Understanding this trajectory shows us just how valuable and impactful Telemedicine is set to become. Slow to change and adapt for decades in the US, healthcare has reached a tipping point of sorts due to COVID-19, with major shortcomings and financial risks of the traditional system exposed. With revenue, financial success, and ultimately our health largely dependent on in-person appointments and globally outsourced supply chains, there is certainly enough momentum for a shift. So what then will our typical healthcare experience look like a year, 3 years, 5 years from now? Sure, we’ll always have needs for direct physical evaluation and care, but with both 5G and Telemedicine ramping up, you can also bet that digital and remote health options are soon to become a major part of our health routine. Will the need (and our preference) be for a 80/20 split of in-person to remote care? 50/50? Or will we move closer to the other end of the spectrum, with preference for remote/online care whenever possible? Whatever the percentages end up looking like, we are now assured that there will be fewer physical touchpoints and more virtual touchpoints in the future.
Impact Now
What then of the now and the immediate future? Returning to a state of financial health and the ability to forecast business operations is now front of mind for every healthcare organization and leader. COVID-19 will continue to have impacts into the foreseeable future, but we’ve created appropriate paths forward even while it remains, and it is time to do the same with financial operating models.
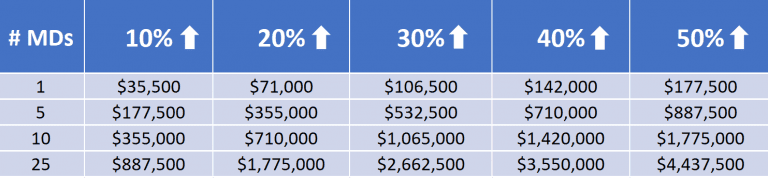
While hospital expectations will shift as well, I comment here specifically with the clinic setting in mind. With the current reimbursement patterns in place for COVID, and assuming a current state 50/50 baseline of in-person to remote care, increasing outpatient telehealth utilization by just 10% equates to about $35,000/yr more, per MD. And while that may not seem like an overly impressive figure, revenue is revenue whether your organization large or small, and that amount reflects a significant reduction in risk as well. While we can’t say it is guaranteed revenue, at this point executing telemedicine visits almost feels like it is, compared to the uncertainty present with elective in-person appointments and no-show rates. Furthermore, as the grid below highlights, those entities with the size and/or opportunity to scale at their advantage really can benefit from a substantial financial tailwind:
Conclusion
Permanency for reasonable compensation and appropriate reimbursement of telehealth related services is on the horizon (Medicare payment bill already underway). Those who plan, prepare, and scale now will have balance sheets and CFOs that thank them.